A systematic review of clinical value of three-dimensional printing in renal disease
Introduction
Three-dimensional (3D) printing has been increasingly used in medicine with reports showing great promise in many areas ranging from applications in orthopaedics and maxillofacial reconstruction to cardiovascular and liver diseases (1-10). Patient-specific 3D printed models based on computed tomography (CT) or magnetic resonance imaging (MRI) data have been shown to accurately replicate complex anatomical structures and pathologies when compared to original source images (2-4,7). 3D printed models can also be used to assist pre-surgical planning and simulation, improve understanding of anatomy and individual lesions (8-10).
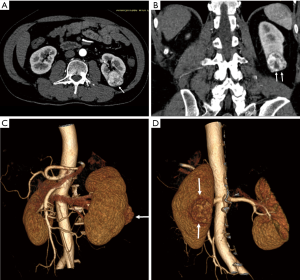
Although two-dimensional (2D) and 3D images are routinely used to diagnose and assess the renal tumours in relation to the surrounding structures prior to surgery (Figure 1), the complex relationships between the renal tumours and different renal structures cannot be fully appreciated on images alone. Further, treatment of renal lesions is moving from traditional open surgery to minimally invasive approach (11-14), thus, it is necessary for surgeons and trainees to obtain a tactile experience of renal tumour or renal system so that better surgical plans or treatment strategies can be determined. Use of 3D printed kidney models in clinical practice fulfils this goal.
Several studies demonstrate the application of 3D printed models in pre-surgical planning of complex renal tumours and renal transplantation (15-18). Despite promising results reported in these studies, there is no systematic review of the current literature about the accuracy of 3D printed models and their clinical applications in renal disease. Thus, the purpose of this review is to analyse current literature with regard to the clinical value of 3D printed models in renal disease, with a focus on application of 3D printed models in renal tumours. Types of 3D printers used for 3D printing, software tools for image post-processing and segmentation, and duration of 3D printing as well as cost associated with 3D printing are also analysed in the review.
Methods
Search strategy
This review was performed to comply with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines (19). A search of two main databases PubMed and Scopus was conducted to identify studies reporting the usefulness of 3D printed models in renal disease. The following keywords were used to perform the search: renal tumours OR renal disease AND 3D printing; renal tumours or renal disease AND 3D printed models; renal tumours OR renal disease AND rapid prototyping; renal tumours OR renal disease AND additive manufacturing; renal tumours OR renal disease AND 3D simulations. The research was limited to peer-reviewed studies published in English within the last 10 years (last search: March, 2018) to ensure the relevance of these studies to the current practice in 3D printing.
Since research on 3D printing in renal disease is at its infancy and the number of studies is limited in the literature, both case reports and original research studies were included in this review to allow systematic analysis of the current research in this area.
Eligibility criteria and data extraction
Two assessors conducted the search of the studies by screening the title and abstract of all identified references independently. Eligible studies must meet the following criteria: either prospective or retrospective studies (case reports, case series or original studies) on patient-specific 3D printed kidney models reporting the clinical value or usefulness of 3D printing in renal anatomy or renal disease. Based on these criteria, review articles, phantom studies, editorials and conference abstracts were excluded. When multiple studies were published by the same research group, details of the study design and findings were checked and duplicate reports were excluded with the most recent ones included in the analysis.
Full texts of the eligible studies were then reviewed and assessed by two assessors independently with agreement reached during discussion. Data extraction includes: accuracy of 3D printed models in delineating renal anatomy and renal tumour, clinical value and usefulness of 3D printed kidney models in pre-surgical planning and simulation of renal procedures; and 3D printed kidney models in patient or medical education. Further, duration of image post-processing and segmentation, software tools used for image processing, types of 3D printers, 3D printing materials and associated costs, and duration of 3D printing were also analysed in the review.
Results
Literature search outcome
The initial search retrieved sixty-one articles. Forty articles were excluded due to their irrelevant to the topic. Of 21 full-text articles that were selected, two were excluded with one being review article and another one technical report. Of 19 eligible studies, 4 were further excluded because of duplicate publication in 2 studies by the same research group (20,21), while another 2 studies focused on 3D printed renal compartments for nuclear medicine imaging without reporting any clinical application of 3D printed models in renal anatomy or renal disease (22,23). Thus, a total of 15 articles were finally included in this review (15-18,24-34). Figure 2 shows the search strategy to identify these eligible studies.
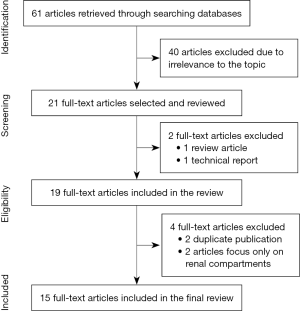
Table 1 is a summary of study characteristics of the use of 3D printed models in renal disease. Of 15 studies, isolated case reports with creation of 1–3 patient-specific 3D printed models were seen in 6 studies, while generation of 5 to 10 3D printed models was reported in 9 studies.
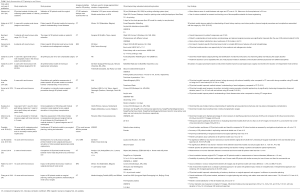
Full table
CT is the most commonly used imaging modality for segmentation of anatomical structures, with 12 studies using CT data as the source of imaging data for 3D printing. MRI data were used in two studies, while in the remaining study, CT or MRI images were used for creating 3D printed models (Table 1).
Quantitative assessment of 3D printed kidney models
Of 15 studies, 8 (53%) provided quantitative assessments of 3D printed kidney models with reported applications in different aspects (16,18,24,29,30,32-34). Comparison of dimensional accuracy or renal tumour volume between 3D printed models and original imaging data/or surgical results was reported in 5 studies (18,24,32-34). Results of these studies showed that 3D printed models are highly accurate in replicating anatomical structures or detecting tumour volumes with mean difference <10% in dimensional measurements between 3D printed models and original imaging data or surgically resected specimens (Table 1).
The other 3 studies reported quantitative assessments of 3D printed models in different perspectives (16,29,30). This includes the following findings: significant reduction in intraoperative ultrasound duration with use of 3D printed models when compared to that without using models (16); medical trainees’ accuracy in nephrectomy score was significantly improved with reduced variability with assistance from 3D printed models in comparison with CT scans (29); 3D printed models assisted medical students, surgeons and radiologists to identify anatomical structures with highest percentage of correct answers, and shorter time spent on recognising anatomy when compared to 3D virtual reconstructions and 2D CT images (30).
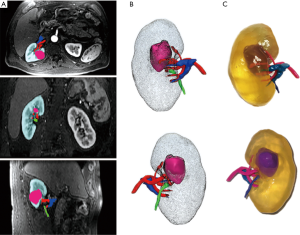
Figures 3-5 are examples of showing patient-specific 3D printed kidney models based on CT or MRI data with excellent demonstration of renal anatomical structures and renal tumours.
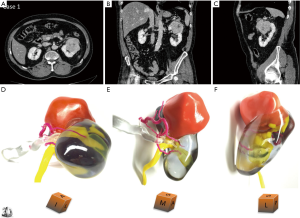
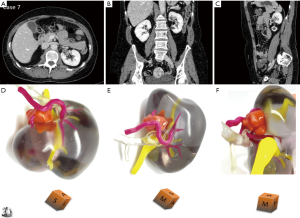
Qualitative assessment of 3D printed kidney models
There are 7 studies reporting the qualitative assessment of 3D printed models in renal disease (15,17,25-28,31). Three of them showed that patient’s understanding of renal anatomy and pathology was improved with use of 3D printed models, with patient’s satisfaction score more than 9 out of 10 (15,25,31). Another three studies demonstrated the clinical value of using 3D printed models in pre-operative planning or simulation of surgical procedures, which led to reduction of surgery duration and intraoperative complications, as well as assisting renal transplantation surgery (17,27,28). The remaining study by Dwivedi et al. presented their first report of correlating 3D printed renal molds with MRI tumour features, with the aim of providing opportunities for future studies of radiomic and radiogenomic analysis of renal tumours (26).
Cost and time associated with 3D printing in kidney models
Different software tools were used in performing image post-processing and segmentation of CT or MRI data, with Mimics and 3D Slicer being the most commonly used software, while details of software packages were not reported in two studies (Table 1). The time spent on image processing and segmentation was only reported in 2 studies as shown in the Table (18,33)).
The cost of 3D printing is reported in 10 studies, ranging from USD$100 to USD$1,000, and this is highly dependent on the materials and the type of 3D printers used for 3D printing. In a recent study, Liu et al. compared the cost and accuracy of 3D printed kidney models using commercial 3D printer with those from home-made 3D printer (33). Authors reported that patient-specific 3D printed models with home-made 3D printer were accurate in demonstrating renal anatomical structures and renal tumours when compared to those from the commercial 3D printer, but at much lower cost (USD$1 vs. USD$ 200 per model).
This review shows a variety of different 3D printers used in printing 3D models, with Objet Connex (Stratasys) as the most common one, which was used in 5 studies. Time taken for 3D printing was available in 10 studies, ranging from 2 to 31 h. The entire process or duration of 3D printing ranged from 2 to 9 days according to some studies in this review (16,24,34).
Discussion
This systematic review analyses 15 studies with regard to the clinical value of 3D printed kidney models, with a summary of the following key findings based on the current literature: first, 3D printed kidney models can be successfully generated with use of CT or MRI data, with high accuracy in reproducing renal anatomy and pathology according to quantitative assessments reported by some studies in the review. Second, 3D printed kidney models could serve as a useful tool in preoperative planning and simulation of complex surgical procedures, thus, reducing the operative duration and potential risks or complications associated with the surgery. Last, 3D printed kidney models improve medical trainees’ understanding of complex renal anatomy and pathology, and patients’ understanding of their disease condition. 3D printed models are also found useful by patients to assist doctor-patient discussion or consultation of clinical cases.
2D and 3D CT or MRI image visualizations are commonly used in the diagnosis of renal tumours, however, to fully understand the relationship between renal tumours and surrounding renal anatomical structures could be a challenging task in some cases. 3D printed physical models are reported to show increasing value in clinical practice which is demonstrated in different medical areas, ranging from accurate delineation of anatomical structures and pathologies to improved understanding of complex anatomy and pathology, assistance in preoperative planning and simulation of surgical procedures and medical education (4-10). Some recent systematic reviews have shown the value of 3D printing in cardiovascular and liver diseases. A systematic review of 48 studies has summarised the findings of using 3D printed models in cardiovascular and cerebrovascular diseases, with high accuracy of 3D printing in reproducing complex cardiac anatomy and pathologies, and usefulness in both education and surgical planning (8). Another recent systematic review of 28 studies focuses on the 3D printing in congenital heart disease (10). Through analysis of case reports and original studies the review further confirms the clinical value of patient-specific 3D printed heart models in preoperative planning and simulation of congenital heart disease treatment and improving medical education and doctor-patient communication.
Two systematic reviews on 3D printing in liver disease are available in the current literature with analysis of 6 and 14 studies, indicating the emerging area of using 3D printing in this field (35,36). Studies reporting the application of 3D printed models in renal disease are similar to those in liver disease. This is confirmed by this review with inclusion of 15 eligible studies. To the best of our knowledge, this is the first systematic review of the clinical application of 3D printed kidney models. Despite limited number of studies reporting quantitative and qualitative assessments of 3D printing in renal disease, this review presents encouraging findings of 3D printed kidney models in demonstrating excellent 3D relationship between renal tumours and adjacent anatomical structures, which plays an important role in surgical planning and simulation, although further studies with inclusion of more cases are needed to confirm these results.
There is no doubt that 3D printed models serve as valuable tools in many applications, however there are challenging issues related to 3D printing such as cost and time of production that need to be resolved. Image post-processing and segmentation of medical imaging data could be time-consuming, especially when dealing with 3D printed heart or liver models due to complex structures in these regions. Further, a number of editing processes are applied to ensure successful 3D printing outcomes (10). For 3D printed heart and liver models, the time spent on image processing and segmentation could be up to 12 and 15 hours respectively, according to the systematic review and other reports (9,10). The whole process of creating a 3D printed liver model could be up to 100 hours, and this does not take into account post-printing work, which could take up to 4–5 days as reported in some studies (37-39). Image post-processing and segmentation of renal CT or MRI data for 3D printing is relatively easier when compared to those for heart or liver 3D printing since the contrast-enhanced renal parenchyma, renal vessels and renal tumours can be easily segmented through automatic or semi-automatic approach. In contrast, some manual editing is required for segmenting cardiac or hepatic structures which could be time-consuming (9,10). In this review, only two studies reported the time spent on image processing and segmentation, however, most of the studies (10 out of 15) reported the time spent on 3D printing. With time spent on after 3D printing taken into account, the whole process could take up to a few days, thus, this long duration of 3D printing process needs to be addressed in future studies to make it a feasible and acceptable tool in clinical practice.
Cost of printing 3D kidney models is another challenge, and this depends on the type of 3D printers and materials used for 3D printing. This review shows that with use of low-cost materials or home-made 3D printers, the cost associated with 3D printed kidney models is less than USD$150, as shown in some studies (25,27,28,33). However, a high quality kidney model printed with flexible materials such as TangoPlus and with different colours to highlight renal tumours and vascular or renal collecting structures can cost up to USD$1,000 (15,16,18,26). Therefore, future research is needed to reduce the costs associated with 3D printed kidney models.
There are some limitations in this review. First, 3D printing in renal disease is an emerging area compared to other medical field such as orthopaedic or cardiovascular applications, thus, only a small number of studies are available in the literature. Of 15 studies included in the review, half of them provided quantitative assessments of 3D printed models in renal disease. Further, the quantitative findings provided by these studies are quite variable as shown in the analysis because they focus on different aspects such as dimensional accuracy and tumour volume measurements. Therefore, more studies are needed to provide further evidence on the accuracy of 3D printed kidney models in replicating both anatomy and pathology. Second, this review shows that most of the studies did not provide information on the time spent on image processing and segmentation, most likely due to the use of different software tools (both commercial and open source software packages) for image processing and segmentation by different research groups. Further, as discussed previously, case reports or case series still dominate the current research of 3D printing in renal disease with 1–3 models reported in 6 studies and 5–10 models in 9 studies. There is a lack of original studies (either retrospectively or prospectively designed studies) looking at the clinical value of 3D printed kidney models, and this should be addressed by future studies. Finally, this review shows that it could take up to 30 h to print a 3D kidney model, and the up to a few days for the entire 3D printing process. Therefore, further improvement on production speed and cost reduction is necessary.
In conclusion, this systemic review analyses 15 studies reporting the clinical value or usefulness of 3D printed kidney models in renal disease with findings showing the feasibility and accuracy of 3D printed kidney models in delineating both anatomical renal structures and pathologies. 3D printed models are shown as useful tools in pre-surgical planning and simulation of renal tumours, in particular in minimally invasive renal nephrectomy of renal tumours. 3D printed models improve patient’s understanding of their renal disease status, and enhance medical trainees’ knowledge of renal malignancy when compared to viewing medical images alone. Future research is required to address the issued related to long duration and high cost associated with 3D printing process. Quantitative and qualitative assessments of clinical value of 3D printed kidney models based on a large cohort of patients are also needed to provide robust evidence on this rapidly growing technique.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Naftulin JS, Kimchi EY, Cash SS. Streamlined, inexpensive 3D printing of the brain and skull. PLoS One 2015;10:e0136198. [Crossref] [PubMed]
- Ho D, Squelch A, Sun Z. Modelling of aortic aneurysm and aortic dissection through 3D printing. J Med Radiat Sci 2017;64:10-7. [Crossref] [PubMed]
- Schmauss D, Haeberle S, Hagl C, Sodian R. Three-dimensional printing in cardiac surgery and interventional cardiology: a single-centre experience. Eur J Cardiothorac Surg 2015;47:1044-52. [Crossref] [PubMed]
- Valverde I, Gomez G, Gonzales A, Suarez-Mejias C, Adsuar AF, Coserria JF, Uribe S, Gomez-Cia T, Hosseinpour AR. Three-dimensional patient-specific cardiac model for surgical planning in Nikaidoh procedure. Cardiol Young 2015;25:698-704. [Crossref] [PubMed]
- Giannopoulos AA, Mitsouras D, Yoo SJ, Liu PP, Chatzizisis YS, Rybicki FJ. Applications of 3D printing in cardiovascular diseases. Nat Rev Cardiol 2016;13:701-18. [Crossref] [PubMed]
- Martelli N, Serrano C, van den Brink H, Pineau J, Prognon P, Borget I, El Batti S. Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery 2016;159:1485-500. [Crossref] [PubMed]
- Jones DB, Sung R, Weinberg C, Korelitz T, Andrews R. Three-dimensional modeling may improve surgical education and clinical practice. Surg Innov 2016;23:189-95. [Crossref] [PubMed]
- Sun Z, Lee S. A systematic review of 3-D printing in cardiovascular and cerebrovascular diseases. Anatol J Cardiol 2017;17:423-35. [PubMed]
- Perica E, Sun Z. Patient-specific three-dimensional printing for pre-surgical planning in hepatocellular carcinoma treatment. Quant Imaging Med Surg 2017;7:668-77. [Crossref] [PubMed]
- Lau I, Sun Z. Three-dimensional printing in congenital heart disease: A systematic review. J Med Radiat Sci 2018. Epub ahead of print. [Crossref] [PubMed]
- Bollens R, Rosenblatt A, Espinoza BP, De Groote A, Quackels T, Roumeguere T, Vanden Bossche M, Wespes E, Zlotta AR, Schulman CC. Laparoscopic partial nephrectomy with “on-demand” clamping reduces warm ischemia time. Eur Urol 2007;52:804-9. [Crossref] [PubMed]
- Gill IS, Eisenberg MS, Aron M, Berger A, Ukimura O, Patil MB, Campese V, Thangathurai D, Desai MM. Zero ischemia” partial nephrectomy: novel laparoscopic and robotic technique. Eur Urol 2011;59:128-34. [Crossref] [PubMed]
- Kaczmarek BF, Tanagho YS, Hillyer SP, Mullins JK, Diaz M, Trinh QD, Bhayani SB, Allaf ME, Stifelman MD, Kaouk JH, Rogers CG. Off-clamp robot assisted partial nephrectomy preserves renal function: a multi institutional propensity score analysis. Eur Urol 2013;64:988-93. [Crossref] [PubMed]
- Kihara K, Koga F, Fujii Y, Masuda H, Takokoro M, Yokoyama M, Matsuoka Y, Numao N, Ishioka J, Saito K. Gasless laparoendoscopic single port clampless sutureless partial nephrectomy for peripheral renal tumors: perioperative outcomes. Int J Urol 2015;22:349-55. [Crossref] [PubMed]
- Bernhard JC, Isotani S, Matsugasumi T, Duddalwar V, Hung A, Suer E, Baco E, Satkunasivam R, Djaladat H, Metcalfe C, Hu B, Wong K, Park D, Nguyen M, Hwang D, Bazargani ST, de Castro Abreu AL, Aron M, Ukimura O, Gill IS. Personalized 3D printed model of kidney and tumor anatomy: a useful tool for patient education. World J Urol 2016;34:337-45. [Crossref] [PubMed]
- Komai Y, Sugimoto M, Gotohda N, Matsubara N, Kobayashi T, Sakai Y, Shiga Y, Saito N. Patient-specific 3-dimensional printed kidney designed for “4D” surgical navigation: A novel aid to facilitate minimally invasive off-clamp partial nephrectomy in complex tumor cases. Urology 2016;91:226-33. [Crossref] [PubMed]
- Kusaka M, Sugimoto M, Fukami N, Sasaki H, Takenaka M, Anraku T, Ito T, Kenmochi T, Shiroki R, Hoshinaga K. Initial experience with a tailor-made simulation and navigation program using a 3-D printer model of kidney transplantation surgery. Transplant Proc 2015;47:596-9. [Crossref] [PubMed]
- Wake N, Rude T, Kang SK, Sfiffelman MD, Borin JF, Sodickson DK, Huang WC, Chandarana H. 3D printed renal cancer models derived from MRI data: application in pre-surgical planning. Abdom Radiol (NY) 2017;42:1501-9. [Crossref] [PubMed]
- Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA. PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 Statement. Syst Rev 2015;4:1. [Crossref] [PubMed]
- Smektala T, Goląb A, Królikowski M, Slojewski M. Low cost silicone renal replicas for surgical training-technical note. Arch Esp Urol 2016;69:434-6. [PubMed]
- Silberstein JL, Maddox MM, Dorsey P, Feibus A, Thomas R, Lee BR. Physical models of renal malignancies using standard cross-sectional imaging and 3-dimensional printers: A pilot study. Urology 2014;84:268-72. [Crossref] [PubMed]
- Woliner-van der Weg W, Deden LN, Meeuwis APW, Koenrades M, Peeters LH, Kuipers H, Laanstgra GJ, Gotthardt M, Slump CH, Visser EP. A 3D-printed anatomical pancreas and kidney phantom for optimizing SPECT/CT reconstruction settings in beta cell imaging using 111In-exendin. EJNMMI Phys 2016;3:29. [Crossref] [PubMed]
- Tran-Gia J, Lassmann M. Optimizing image quantification for Lu-177 SPECT/CT based on a 3D printed 2-compartment kidney phantom. J Nucl Med 2018;59:616-24. [Crossref] [PubMed]
- Adams F, Qiu T, Mark A, Fritz B, Kramer L, Schlager D, Wetterauer U, Miernik A, Fischer P. Soft 3D-printed phantom of the human kidney with collecting system. Ann Biomed Eng 2017;45:963-72. [Crossref] [PubMed]
- Atalay HA, Canat HL, Ulker V, Alkan I, Ozkuvanci U, Altunrende F. Impact of personalized three-dimensional (3D) printed pelvicalyceal system models on patient information in percutaneous nephrolithotripsy surgery: a pilot study. Int Braz J Urol 2017;43:470-5. [Crossref] [PubMed]
- Dwivedi DK, Chatzinoff Y, Zhang Y, Yuan Q, Fulkerson M, Chopra R, Brugarolas J, Cadeddu JA, Kapur P, Pedrosa I. Development of a patient-specific tumor mold using magnetic resonance imaging and 3-dimensional printing technology for targeted tissue procurement and radiomics analysis of renal masses. Urology 2018;112:209-14. [Crossref] [PubMed]
- Golab A, Slojewski M, Brykczynski M, Lukowiak M, Boehlke M, Matias D, Smektala T. Three-dimensional printing as an interdisciplinary communication tool: preparing for removal of a giant renal tumor and atrium neoplastic mass. Heart Surg Forum 2016;19:E185-6. [Crossref] [PubMed]
- Golab A, Smektala T, Kaczmarek K, Stamirowski R, Hrab M, Slojewski M. Laparoscopic partial nephrectomy supported by training involving personalized silicone replica poured in three-dimensional printed casting mold. J Laparoendosc Adv Surg Tech A 2017;27:420-2. [Crossref] [PubMed]
- Knoedler M, Feibus AH, Lange A, Maddox MM, Ledet E, Thomas R, Silberstein JL. Individualized physical 3-dimensional kidney tumor models constructed from 3-dimensional printers result in improved trainee anatomic understanding. Urology 2015;85:1257-61. [Crossref] [PubMed]
- Marconi S, Pugliese L, Botti M, Peri A, Cavazzi E, Latteri S, Auricchio F, Pietrabissa A. Value of 3D printing for the comprehension of surgical anatomy. Surg Endosc 2017;31:4102-10. [Crossref] [PubMed]
- Porpiglia F, Bertolo R, Checcucci E, Amparore D, Autorino R, Dasgupta P, Wiklund P, Tewari A, Liatsikos E, Fiori C. The ESUT Research Group. Development and validation of 3D printed virtual models for robot-assisted radical prostatectomy and partial nephrectomy: urologists' and patients' perception. World J Urol 2018;36:201-7. [Crossref] [PubMed]
- von Rundstedt FC, Scovell JM, Agrawal S, Zaneveld J, Link RE. Utility of patient-specific silicone renal models for planning and rehearsal of complex tumour resections prior to robot-assisted laparoscopic partial nephrectomy. BJU Int 2017;119:598-604. [Crossref] [PubMed]
- Liu D, Sun Z, Chaichana T, Ducke W, Fan Z. Patient-specific 3D printed models of renal tumours using home-made 3D printer in comparison with commercial 3D printer. J Med Imaging Health Inf 2018;8:303-8. [Crossref]
- Zhang Y, Ge H, Li N, Yu C, Guo H, Jin S, Liu J, Na Y. Evaluation of three-dimensional printing for laparoscopic partial nephrectomy of renal tumors: a preliminary report. World J Urol 2016;34:533-7. [Crossref] [PubMed]
- Soon DSC, Chae MP, Pilgrim CHC, Rozen WM, Spychal RT, Hunter-Smith DJ. 3D hepatic modelling for preoperative planning of hepatic resection: a systematic review. Ann Med Surg (Lond) 2016;10:1-7. [Crossref] [PubMed]
- Witowski JS, Coles-Black J, Zuzak TZ, Pedziwiatr M, Chuen J, Major P, Budzyriski A. 3D printing in liver surgery: a systematic review. Telemed J E Health 2017;23:943-7. [Crossref] [PubMed]
- Witowski JS, Pędziwiatr M, Major P, Budzyński A. Cost-effective, personalized, 3D-printed liver model for preoperative planning before laparoscopic liver hemihepatectomy for colorectal cancer metastases. Int J Comput Assist Radiol Surg 2017;12:2047-54. [Crossref] [PubMed]
- Igami T, Nakamura Y, Hirose T, Ebata T, Yokoyama Y, Sugawara G, Mizuno T, Mori K, Nagino M. Application of a three-dimensional print of a liver in hepatectomy for small tumors invisible by intraoperative ultrasonography: Preliminary experience. World J Surg 2014;38:3163-6. [Crossref] [PubMed]
- Javan R, Herrin D, Tangestanipoor A. Understanding spatially complex segmental and branch anatomy using 3D printing: liver, lung, prostate, coronary arteries, and circle of willis. Acad Radiol 2016;23:1183-9. [Crossref] [PubMed]


