
Quality and accuracy of 3D printed models in medicine
We have observed the increasing interest of QIMS journal in 3D printed models applied to medicine. We have been working with this technology since 2011 and we have manufactured more than 500 3D printed models for surgical planning and medical applications. We have read the original article by Allan et al. (1) with a considerable interest because the authors are investigating new clinical areas such as biliary disease.
The authors found significant differences in measurements between the standard tessellation language (STL) and original computed tomography (CT) images, and also between the 3D printed models and the original CT images.
In our experience these deviations may be related to the computer aided design (CAD) operations with the STL file in order to obtain a model suitable for 3D printing.
When we are trying to print hollow models, the clinicians have to define the volume of interest. As we can observe in the images of the article, the tubular structures of the biliary conduct are collapsed. This deformation occurs when an offset operation is applied to the original mesh. The smaller the structures and the higher the thickness the easier is to have misrepresentations of the real anatomy.
There are several ways to minimize these problems. First option is reducing the wall thickness. This is not an easy operation because depending on the material and the 3D printer used, creating models with walls thinner than 1 mm is really difficult. We have been working with Filaflex (Recreus, Spain) flexible filaments and fused deposition modeling printers and we have been able to print congenital heart disease models with 0.4 mm wall thickness (Figure 1).
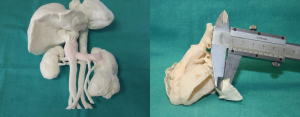
Second option is modifying the offset direction. If we are interested in the inner part of the model, offset operation has to be performed normally. For example, we have manufactured this kind of models when we have used them to plan cardiac catheterization and surgical interventions (2-5). In these cases, the comparison between CT images and 3D printed models has to be made measuring the inner surface.
When the external surface of the model is the area of interest the offset operation has to be inverted, reducing the volume inside the model. In this case, the comparison between CT images and 3D printed models has to be made measuring the outer surface.
As we have studied and demonstrated, the accuracy of 3D printed models is more affected for the segmentation and CAD processes than for the 3D printing itself (2,5).
We have experience collaborating with different medical specialties such as plastic surgery, maxillofacial surgery, traumatology, oncological surgery, urology, cardiac surgery, etc.
In conclusion, we would like to affirm that 3D printed models provide a great added value to the clinical practice, improving the quality of care and the communication with patients and their families.
Acknowledgments
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Allan A, Kealley C, Squelch A, Wong YH, Yeong CH, Sun Z. Patient-specific 3D printed model of biliary ducts with congenital cyst. Quant Imaging Med Surg 2019;9:86-93. [Crossref] [PubMed]
- Valverde I, Gomez G, Coserria JF, Suarez-Mejias C, Uribe S, Sotelo J, Velasco MN, Santos De Soto J, Hosseinpour AR, Gomez-Cia T. 3D printed models for planning endovascular stenting in transverse aortic arch hypoplasia. Catheter Cardiovasc Interv 2015;85:1006-12. [Crossref] [PubMed]
- Dubois D, Vaquerizo B, Valverde I, Escabias C, Gomez G, RodriguezCollado J, Zunzunegui JL, Freixa X, Barreiro-Perez M, Suarez-Mejias C, Alcalde O, Cruz-Gonzalez I. Percutaneous left atrial appendage closure guided by 3D-printed cardiac model. Eur Heart J 2017;38: ehx493.P6092.
- Valverde I, Gomez G, Gonzalez A, Suarez-Mejias C, Adsuar A, Coserria JF, Uribe S, Gomez-Cia T, Hosseinpour AR. Three-dimensional patient-specific cardiac model for surgical planning in Nikaidoh procedure. Cardiol Young 2015;25:698-704. [Crossref] [PubMed]
- Valverde I, Gomez-Ciriza G, Hussain T, Suarez-Mejias C, Velasco-Forte MN, Byrne N, Ordoñez A, Gonzalez-Calle A, Anderson D, Hazekamp MG, Roest AAW, Rivas-Gonzalez J, Uribe S, El-Rassi I, Simpson J, Miller O, Ruiz E, Zabala I, Mendez A, Manso B, Gallego P, Prada F, Cantinotti M, Ait-Ali L, Merino C, Parry A, Poirier N, Greil G, Razavi R, Gomez-Cia T, Hosseinpour AR. Three-dimensional printed models for surgical planning of complex congenital heart defects: an international multicentre study. Eur J Cardiothorac Surg 2017;52:1139-48. [Crossref] [PubMed]


