The evaluation of spontaneous Descemet’s membrane reattachment using swept-source optical coherence tomography: a case report
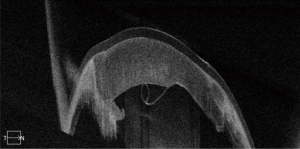
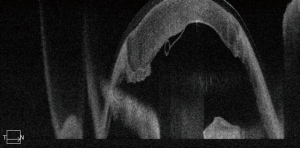
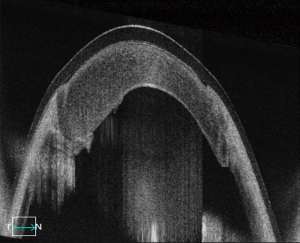
A 29-year-old man presented with a history of facial burn in August of 2017. Slit lamp examination revealed significant central corneal stromal scarring in the right eye. The patient received deep anterior lamellar keratoplasty (DALK) in the right eye. Three weeks post operatively, the patient was found to have recurrent corneal edema on slit lamp exam, and standard anterior segment optical coherence tomography (OCT) revealed a central detachment of Descemet’s membrane. An air bubble was introduced into the anterior chamber. However, 1 week following the procedure, the corneal edema persisted, and standard OCT had insufficient view of the structural details. Swept-source OCT (SS-OCT, PLEX® Elite 9000; Carl Zeiss Meditec, Inc., Dublin, CA, USA) (1) was then performed to further examine the depth and detail of the detachment, revealing an inferior Descemet’s detachment (Figure 1). Observation was elected and sequential imaging studies with SS-OCT were planned to guide further intervention. One month later, SS-OCT imaging revealed signs of reattachment (Figure 2) and by two months, the membrane had completely reattached (Figure 3).
Corneal endothelial cell layer is critical to control corneal edema and ensure the clarity. In some cases following DALK, the host endothelial layer (with its basement membrane, Descemet’s membrane) may be detached from the donor tissue, causing significant edema. Descemet’s detachment treatments include observation, the introduction of an air bubble into the anterior chamber, surgical suturing, or keratoplasty (2). Many cases of spontaneous reattachment have been reported, highlighting the value of conservative treatment. Diagnosis and treatment decisions of a Descemet’s detachment is often based on clinical exam (slit lamp) in combination with quality imaging (such as standard anterior segment OCT) (3-6). However, in severe case of corneal edema, both slit lamp and standard anterior segment OCT may be challenging.
SS-OCT is a useful imaging technique for the anterior segment imaging due to its unique advantages. SS-OCT has a central wavelength of 1,060 nm, producing an A-scan depth of 3 mm, while standard anterior segment OCT device, which is based on spectral domain configuration (SD-OCT), has a shorter central wavelength of 830 nm and produces a limited A-scan depth of 1.8 mm. In addition, SS-OCT equips with a faster scanning rate of 100 kHz compared to the 20–40 kHz speeds of SD-OCT. Due to the longer wavelength and faster scanning speed, the SS-OCT provides deeper penetration, shows higher image quality, and demonstrates a wider view of the microstructure of the eye compared to current SD-OCT, as demonstrated by the wide and full structural views of the Descemet’s membrane detachment and spontaneous reattachment presented here. In this case, we used SS-OCT to visualize the detachment of Descemet’s membrane and follow the progression of its spontaneous reattachment, sparing the patient from any further invasive treatments. Thus, SS-OCT can be a useful tool for the diagnosis and follow-up of various ocular conditions, as demonstrated by this case of spontaneous Descemet’s reattachment.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Miller AR, Roisman L, Zhang Q, Zheng F, Rafael de Oliveira Dias J, Yehoshua Z, Schaal KB, Feuer W, Gregori G, Chu Z, Chen CL, Kubach S, An L, Stetson PF, Durbin MK, Wang RK, Rosenfeld PJ. Comparison Between Spectral-Domain and Swept-Source Optical Coherence Tomography Angiographic Imaging of Choroidal Neovascularization. Invest Ophthalmol Vis Sci 2017;58:1499-505. [Crossref] [PubMed]
- Chow VW, Agarwal T, Vajpayee RB, Jhanji V. Update on diagnosis and management of Descemet’s membrane detachment. Curr Opin Ophthalmol 2013;24:356-61. [Crossref] [PubMed]
- Lin X, Wu Y, Fu Y, Dai Q. Spontaneous reattachment of Descemet membrane detachment after deep anterior lamellar keratoplasty: A case report. Medicine (Baltimore) 2018;97:e0032. [Crossref] [PubMed]
- Tu KL, Ibrahim M, Kaye SB. Spontaneous resolution of Descemet membrane detachment after deep anterior lamellar keratoplasty. Cornea 2006;25:104-6. [Crossref] [PubMed]
- Marcon AS, Rapuano CJ, Jones MR, Laibson PR, Cohen EJ. Descemet’s membrane detachment after cataract surgery: management and outcome. Ophthalmology 2002;109:2325-30. [Crossref] [PubMed]
- Patel DV, Phang KL, Grupcheva CN, Best SJ, McGhee CN. Surgical detachment of Descemet's membrane and endothelium imaged over time by in vivo confocal microscopy. Clin Exp Ophthalmol 2004;32:539-42. [Crossref] [PubMed]