An unusual complication of dermatillomania
Dermatillomania or skin picking disorder (sometimes called excoriation disorder, neurotic picking, psychogenic excoriation) is characterized by repetitive skin picking leading to tissue damage. Skin picking may result in significant tissue damage and often leads to medical complications such as localized infections. We present a case of a patient who presented with bacteremia, an extensive workup failed to identify the source of bacteremia. However, skin examination findings helped to identify the source, which was attributed to skin infection secondary to skin picking disorder.
A 54-year-old African American male, with a past medical history of diabetes mellitus, presented with generalized fatigue and fever. Physical examination was significant for hypotension and tachycardia. Skin exam showed multiple hyperkeratotic hyperpigmented lesions, mainly on posterior neck and forearms. It was also notable for bilateral fingertips thinning and lacerations with surrounding edema and areas of focal skin necrosis (Figure 1). He did not show any abnormalities suggestive of neuropathy. Blood cultures showed persistent staphylococcus aureus bacteremia. Extensive workup for the source of bacteremia (including bone X-ray, transesophageal echocardiogram, and chest CT scan) was negative, an extensive workup for immunodeficiency was also negative (including HIV, leukocyte count and CD4 count, immunoglobulin assay, autoimmune workup, as well as nitro blue tetrazolium test). The source of bacteremia was attributed to skin infection secondary to skin picking disorder. On further questioning, patient showed obsessive compulsive like behavior in picking on his skin, with previous failed attempts to alleviate his behavior mainly by covering his hand using gloves. The patient has never had any skin infections before, he reported repeated thoughts of picking on skin edges and removing minor skin irregularities, while recognizing that it could be harmful to his health, but he continued to do it as it provided relief and upon reasoning he stated “this happens with age, I started doing that when I got older and I cannot stop doing it”. Patient met DSM-5 diagnostic criteria for excoriation skin picking disorder and was referred to outpatient psychiatry unit, patient did not have any other psychiatric illness or drug abuse. The patient’s condition improved significantly with psychotherapy, and his skin lesions also improved.
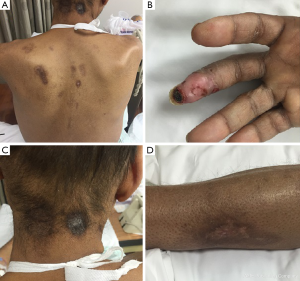
Dermatillomania or skin picking disorder is characterized by repetitive skin picking leading to tissue damage. Skin picking disorder can lead to serious medical conditions, such as Scarring, ulcerations and infections (1).
Despite a lifetime prevalence of 1.4% in general population, Skin picking disorder is believed to be underreported. It is more commonly reported in females, with a median age of onset of 30–45 years (2,3). Due to its relative high prevalence and morbidity, it has been included lately in DSM-5. Neurotic excoriations are due either to an underlying psychopathology or to the formation of habit. Accordingly, their pathophysiology is poorly understood (4).
The following diagnostic criteria have been proposed and studied in a field trial for dermatillomania: (I) recurrent skin picking resulting in skin lesions; (II) repeated attempts to decrease or stop skin picking; (III) the skin picking causes clinically significant distress or impairment in social, occupational, or other important areas of functioning; (IV) the skin picking is not attributable to the direct physiological effects of a substance (e.g., cocaine) or another medical condition (e.g., scabies); and (V) the skin picking is not better accounted for by symptoms of another DSM-5 disorder (e.g., skin picking due to delusions or tactile hallucinations in a psychotic disorder, preoccupation with appearance in body dysmorphic disorder) (1,5).
Skin picking may result in significant tissue damage and often leads to medical complications such as localized infections. The repetitive, excoriation nature of picking in severe cases may even warrant skin grafting (6,7). Skin is one of the sources for Staphylococcal infection, our case presents a patient with Staphylococcus aureus bacteremia secondary to skin infection related to skin picking disorder.
This case report illustrates the importance of skin examination and the recognition of skin findings in patients with skin picking disorder which is frequently underdiagnosed. Early diagnosis and appropriate treatment by physicians are essential to prevent potentially fatal consequences.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Arnold LM, Auchenbach MB, McElroy SL. Psychogenic excoriation. Clinical features, proposed diagnostic criteria, epidemiology and approaches to treatment. CNS Drugs 2001;15:351-9. [Crossref] [PubMed]
- Grant JE, Stein DJ, Woods DW, Keuthen NJ. Trichotillomania, Skin Picking, and Other Body-Focused Repetitive Behaviors. American Psychiatric Publishing. 2011.
- Hayes SL, Storch EA, Berlanga L. Skin picking behaviors: An examination of the prevalence and severity in a community sample. J Anxiety Disord 2009;23:314-9. [Crossref] [PubMed]
- Keuthen NJ, Koran LM, Aboujaoude E, Large MD, Serpe RT. The prevalence of pathologic skin picking in US adults. Compr Psychiatry 2010;51:183-6. [Crossref] [PubMed]
- Diagnostic and Statistical Manual of Mental Disorders (DSM–5). Available online: www.DSM5.org
- Lochner C, Simeon D, Niehaus DJ, Stein DJ. Trichotillomania and skin-picking: a phenomenological comparison. Depress Anxiety 2002;15:83-6. [Crossref] [PubMed]
- Wilhelm S, Keuthen NJ, Deckersbach T, Engelhard IM, Forker AE, Baer L, O'Sullivan RL, Jenike MA. Self-injurious skin picking: clinical characteristics and comorbidity. J Clin Psychiatry 1999;60:454-9. [Crossref] [PubMed]


