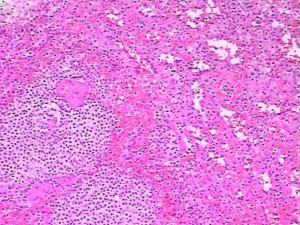
Planted spleen fragments misdiagnosed as hepatic cancer
A 61-year-old man, who had hepatitis B for many years, presented for a routine abdominal examination and a liver mass was found by the routine B-mode ultrasound examination. Five years ago the patient received splenectomy for a traumatic splenic rupture and the mass was the spleen fragments which were planted in the liver, but the patient was initially misdiagnosed as liver cancer.
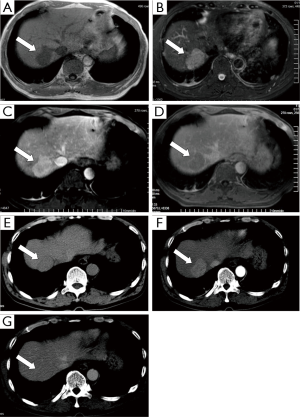
The patient had no complaint of abdominal pain, bloating and nausea, no symptoms of haematemesis, vomiting, melena or yellow eyes. He had good sleep and appetite, and no significant weight loss. His stool and urine examinations were normal. Physical scleral jaundice was negative and the liver was not palpable under the costal margin; he had no percussion pain, and ascites was negative. Serum biomarkers shows CEA 3.93 ng/mL (local reference range: 0-10 ng/mL), CA199 3.50 U/mL (local reference range: 0-39 U/mL), and AFP 2.69 ng/mL (local reference range: 0-10 ng/mL). Abdominal MR and CT diagnosed the patient had hepatic cancer (Figure 1). Preoperative diagnosis: 1. Liver mass: hepatic cancer? 2. Post splenectomy changes.
A laparotomy was performed under general anesthesia. A protruding liver mass close to adhesions around the diaphragm was found in segment VII. The mass was about the size of 25.0 mm × 40.0 mm, with a hard texture and unclear boundary with the surrounding liver. During the operation a quick frozen pathology showed it was residual spleen tissue (Figure 2). The resection of liver mass continued. After surgery, the patient was injected with ceftriazone against infection for two days. The patient had a good recovery, and the stitches were removed on the 10th day. Follow-up for the patient was uneventful.
Acknowledgements
Disclosure: The author declares no conflict of interest.