Fracture and atypical migration of an implantable central venous access device
Introduction
Central venous catheter device (CVC) is often implanted in the purpose of delivering parenteral chemotherapy or nutrition. Thrombosis and infection are well-known complications of these devices. However, pinch-off syndrome (POS) is less common but severe. We report a case of POS with an atypical migration.
Case presentation
A 52-year-old woman diagnosed with a right breast cancer had undergone conservative surgery in July 2015. A CVC was inserted through the left subclavian vein in February 2015 for adjuvant chemotherapy, and the location was confirmed by chest X-ray. The cycles of chemotherapy were administered without any trouble, pain or swelling.
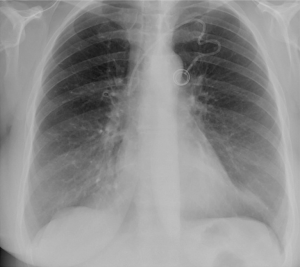
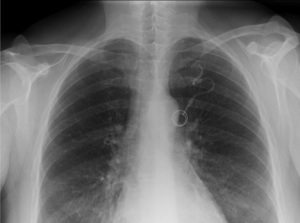
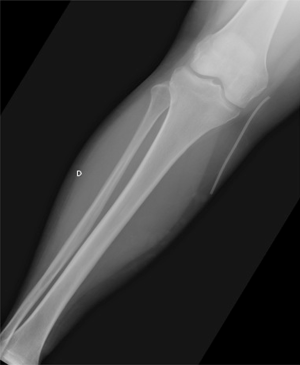
Six months after the CVC implantation, the patient suffered from an anterior thoracic trauma on her left side due to a domestic accident. The chest X-ray made at that moment revealed that the extremity of the catheter was in place in the superior vena cava (Figure 1), and remained stable compared to the first control. However, the grade 1 of the POS was not diagnosed: there was an atypical course with abrupt change in direction. In November, three months later, the patient was addressed to the hospital by her general physician because of a cough resistant to the medical treatment. A chest X-ray was performed and showed normal lung fields, but revealed a shortened catheter and no tip was seen in the heart cavities or pulmonary artery projection (Figure 2). Further exams were performed in order to find the tip of the catheter: chest and abdominal CT scan, neck X-ray, and heart echography. The fractured part of the catheter was not seen. Finally, the missed catheter was found on lower limbs X-ray on the internal side of the right knee, and appeared to be superficial (Figure 3). The patient was referred to a surgeon and the migrated catheter was successfully removed from the long saphenous vein via a small incision. The remaining implantable venous port was removed at the same time.
Discussion
The typical complications with venous access ports are venous thrombosis, port infection, extravasation, and occlusion. POS with intravenous catheter fracture and migration is rare with a reported incidence of 0.1–1% (1). This syndrome was described by Aitken et al. in 1984, and is characterized by intermittent catheter malfunction in conjunction with radiologic evidence of catheter compression between clavicle and first rib (2). A radiological scale of catheter distortion was defined by Hinke et al. (3): grade 0, no compression and distortion; grade 1, no luminal catheter narrowing but deviation; grade 2, luminal narrowing as the catheter passes under the clavicle (true pinch-off sign); and grade 3 defines complete catheter transection and embolization of the distal catheter. Unfortunately, this radiographic grading is not incorporated into daily clinical practice. In the literature, the average length of time between catheter insertion and fracture was between 5.3 and 6.7 months (4,5).
The most common clinical presentations are pain with or without swelling at the insertion site, dysfunctional catheter and problems with blood aspiration or flushing. The less common are accidental discovery of catheter embolization on routine chest X-ray, cardiac palpitation, bilateral chest pain, abdominal pain and nausea, new S3 heart sound, paresis of the ipsilateral arm (4). The main cause of catheter transection is the POS due to chronic compression between the clavicle and the first rib on the surrounding connective tissue of the subclavian vein. In most cases the tip of the catheter is discovered in the heart cavities or pulmonary artery. In our case, the POS wasn’t diagnosed. The implication of the thoracic trauma is unclear. The migration site is very atypical and the mechanism is not established. Our hypothesis is that the fragmented catheter would have to pass through the superior vena cava into inferior vena cava, and further against the current of the blood flow towards the iliac veins, femoral veins and stopped into the saphenous vein. The superficial localization of the fragmented catheter allowed us to perform surgery with a small incision on the popliteal region to remove the catheter. Usually, removal of the migrated fragments into heart cavities or pulmonary artery is performed by angiographic intervention through a femoral vein approach and only occasionally by open thoracotomy.
In conclusion, the particularity of this interesting POS case is the atypical migration into the saphenous vein, without any clinical symptoms. We conclude that in cases of catheter narrowing, patients should be followed carefully by repeated chest X-ray, in order to prevent and early detect the POS and remove the CVC immediately if no longer required. To avoid POS, theoretically a catheter must be inserted into the subclavian vein as laterally as possible (6).
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Kim OK, Kim SH, Kim JB, Jeon WS, Jo SH, Lee JH, Ko JH. Transluminal removal of a fractured and embolized indwelling central venous catheter in the pulmonary artery. Korean J Intern Med 2006;21:187-90. [Crossref] [PubMed]
- Aitken DR, Minton JP. The "pinch-off sign": a warning of impending problems with permanent subclavian catheters. Am J Surg 1984;148:633-6. [Crossref] [PubMed]
- Hinke DH, Zandt-Stastny DA, Goodman LR, Quebbeman EJ, Krzywda EA, Andris DA. Pinch-off syndrome: a complication of implantable subclavian venous access devices. Radiology 1990;177:353-6. [Crossref] [PubMed]
- Mirza B, Vanek VW, Kupensky DT. Pinch-off syndrome: case report and collective review of the literature. Am Surg 2004;70:635-44. [PubMed]
- Nace CS, Ingle RJ. Central venous catheter "pinch-off" and fracture: a review of two under-recognized complications. Oncol Nurs Forum 1993;20:1227-36. [PubMed]
- Magney JE, Staplin DH, Flynn DM, Hunter DW. A new approach to percutaneous subclavian venipuncture to avoid lead fracture or central venous catheter occlusion. Pacing Clin Electrophysiol 1993;16:2133-42. [Crossref] [PubMed]